By Alex LaTrenta, Greenwich Academy class of 2020
Second in a series of articles about the prevention, recognition, and treatment of public health threats in Greenwich
The elderly man lay motionless on the table unable to speak, his right side paralyzed by a devastating, acute stroke. Dr. Matouk, Chief of Neurovascular Neurosurgery at Yale, threaded a tube under local anesthesia through a major leg artery into his brain, pulling out the clot causing the stroke. Within minutes, the patient began moving his right side again and went from a future of disability to having the potential to live a normal life. By the end of the year, this scenario could occur with frequency at Greenwich Hospital where onsite neurointerventional physicians can perform this life-saving procedure right in our community.
While everyone knows that crushing chest pain radiating to the left arm might indicate a heart attack, many people think that paralysis on one side of the body is the only symptom of an acute stroke. In reality, sudden loss of vision in one eye, numbness or tingling in an arm or leg, word-finding difficulty, imbalance and dizziness could all be signs of a stroke.
People need to start thinking of strokes as “brain attacks” and learn to recognize the signs and symptoms because prompt medical attention and modern techniques at the Greenwich Hospital Stroke Center can prevent or reverse brain damage.
Strokes are a major cause of death and disability in the United States: 1 out of 20 deaths occur from stroke and every 40 seconds someone has a stroke. Strokes kill twice as many women as breast cancer and are the number one cause of long term disability regardless of gender. The risk increases several fold for people with high blood pressure (hypertension), diabetes, or a history of smoking.
Strokes occur when a blood clot blocks flow to the brain or when an artery in the brain bursts; this interruption of oxygen to the brain results in cell death or dysfunction. The sooner the circulation can be restored, the less brain damage occurs. It is a common misconception that stroke symptoms are not an emergency because there is no way to treat a stroke. The opposite is true— every second counts, especially since novel stroke treatments to dissolve or extract blood clots are available.
Not all strokes occur without warning as some people have a transient ischemic attack (TIA) but might not recognize the significance. These episodes of stroke-like symptoms—transient vision loss, momentary confusion, loss of speech, or weakness/numbness—can last 5 minutes or longer but resolve completely on their own. More than a third of people who have a TIA and do not seek treatment suffer a major stroke within one year.
Greenwich residents must be vigilant about any stroke symptoms no matter how brief and seek emergency treatment. Dr. Chris Davison, Director of Emergency Medicine at Greenwich Hospital (GH), recommends using the BEFAST acronym to recognize a stroke in yourself or a loved one:
Balance = Sudden loss of balance?
Eyes = Loss of vision in one or both eyes?
Face = Looks uneven?
Arm = (or leg) Weak or hanging down?
Speech = Slurred words, trouble speaking, or disoriented?
Terrible headache and time = Call 911 immediately!
Davison advises that “patients should not wait to see if symptoms improve. They should seek medical attention immediately as certain treatments are time sensitive.” If family or friends are present, they should note the exact time of symptom onset or the last time the person was seen without symptoms.
If a stroke occurs, do not drive or have another person drive to the Emergency Room (ER); call 911 immediately. Given that GH is a stroke center, Davison explains that the ambulance personnel “can evaluate and assess patients and if they deem that the patient is having a stroke, they can initiate the stroke alert notification process prior to the patient even arriving in the Emergency Department.”
The town of Greenwich is fortunate that Greenwich Hospital was the first healthcare facility in Fairfield County to earn national certification as a primary stroke center. Patients in Greenwich have access to the highest standard of care and the latest treatment protocols.
Once medical professionals determine that a patient is having a stroke, they activate the stroke alert system which summons a neurologist to the ER and notifies the technologist operating the CT scanner in the ER. If the stroke symptoms occurred within 4.5 hours of arrival, a patient may be eligible to receive clot-dissolving (thrombolytic) medications such as tissue plasminogen activator (tPA) or alteplase. Used since the 1990s with great success, these medications work to unblock the blood vessels in the brain and restore blood flow.
Along with a regular CT scan of the brain, a stroke alert patient will receive a specialized CT scan called a CT angiogram to inspect all of the major blood vessels in the head and neck for a blood clot in a large vessel.
Approximately 15 to 20 percent of patients have blockages of major arteries in the brain which may not resolve with clot-dissolving medications alone and often have worse clinical outcomes. In these patients, neurovascular surgeons can insert a tube under local anesthesia through a large artery in the leg and thread it up into the brain to pull out the clot and restore blood flow.
When discussing which patients are eligible for this novel therapy, Matouk explains “ if it’s a large vessel then we can go after it. If it’s a small vessel somewhere far away …we typically won’t chase those.”
Patients with large vessel blockage can benefit from this interventional procedure even 6 to 24 hours after the onset of stroke symptoms resulting in less brain damage and/or cell death. Currently these patients must be transported to Yale for this procedure; however, Matouk revealed that “by the beginning of December, we should have a 24/7 thrombectomy program at Greenwich Hospital. “
As the President of Greenwich Hospital Norman Roth declared, “Greenwich Hospital’s investment in neuroscience will soon provide life-saving thrombectomies for patients presenting with aneurysms and blockages from stroke. This life-saving treatment can preserve brain function and prevent serious injury or death allowing the patient to go on with their life after a critical incident.”
By knowing how to recognize either TIA or stroke symptoms and seeking prompt medical attention at the Greenwich Hospital Stroke Center, residents can save lives and decrease disability within the Greenwich Community.
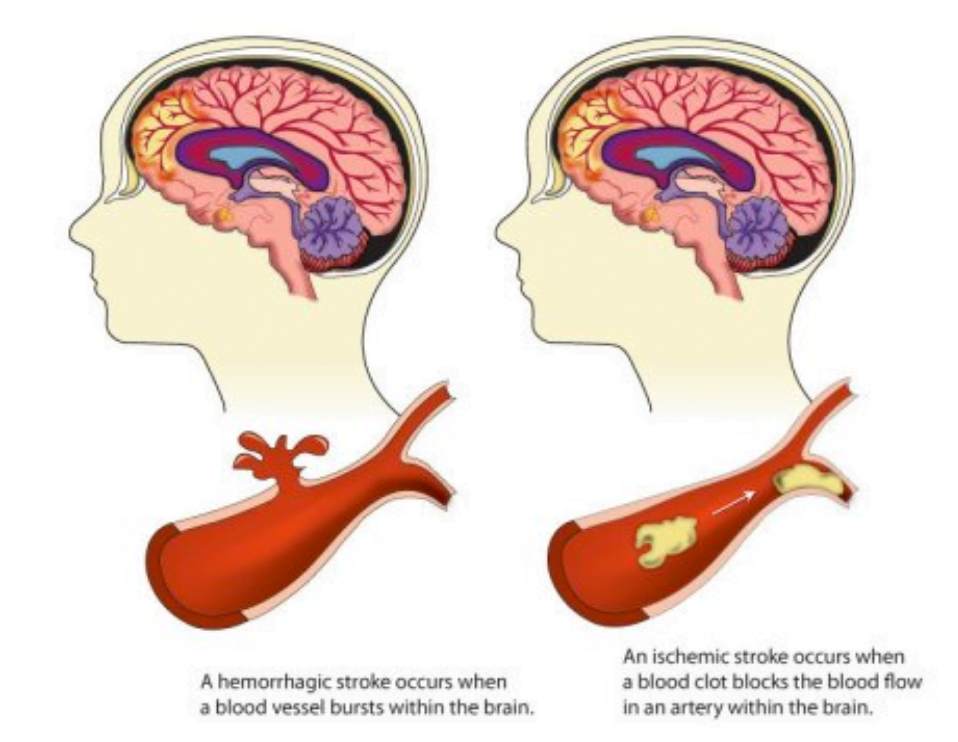
^CDC website: 85% of strokes are ischemic strokes which might be eligible for clot-dissolving medications or mechanical clot removal while 15% are hemorrhagic
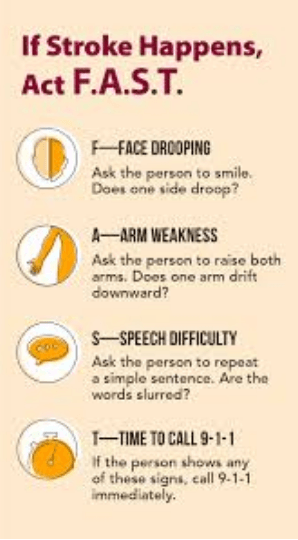
^CDC website: Recognition of stroke symptoms—Every second counts.
Interview of Dr. Matouk Chief of Neurovascular Neurosurgery at Yale and a stroke patient.